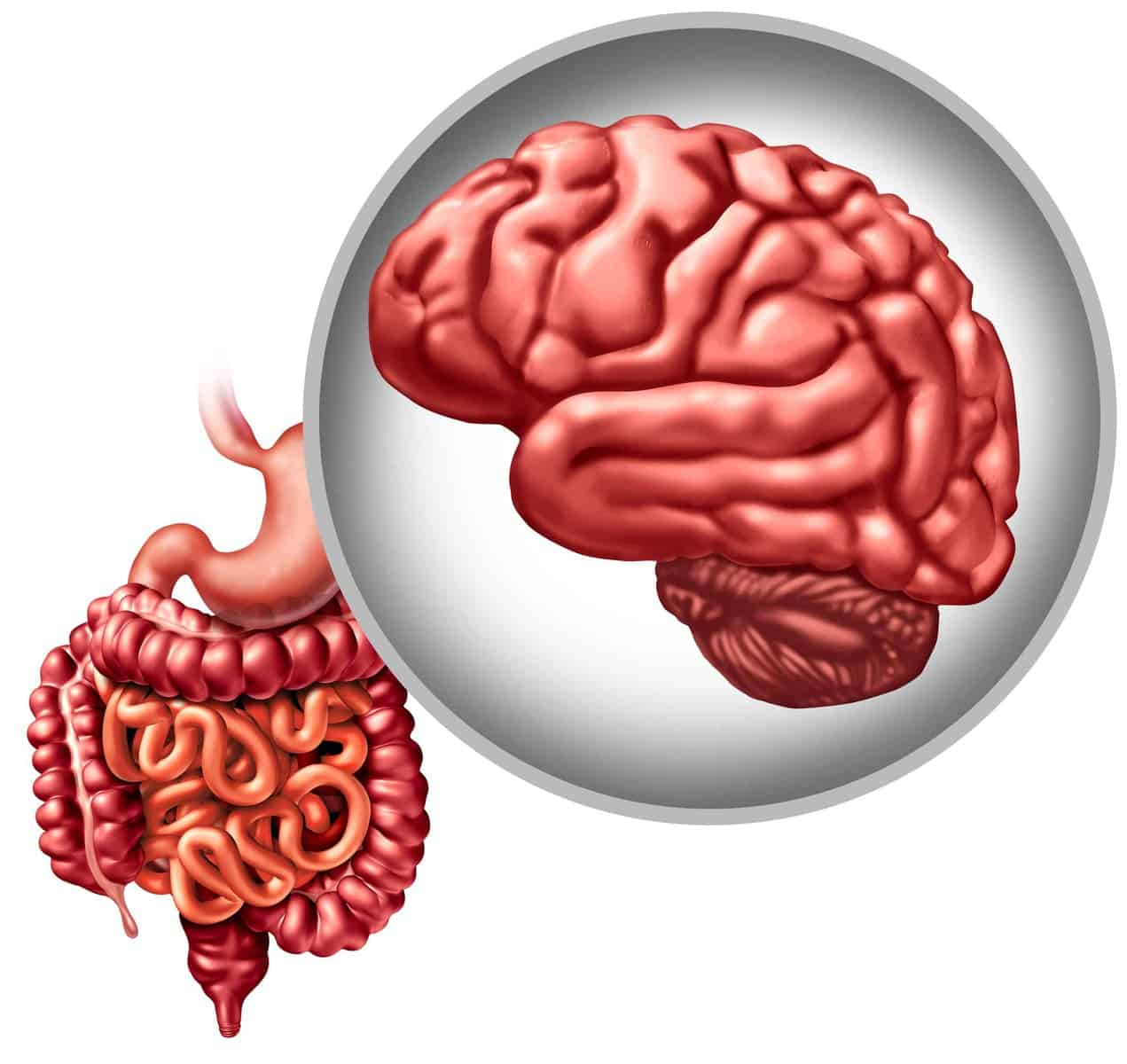
Your brain and your gut share something beyond a metaphorical connection: they’re protected by nearly identical barrier systems that break down through the same mechanisms. When your gut barrier fails, allowing bacterial toxins and inflammatory molecules into circulation, those same molecules attack the blood-brain barrier. The result is a cascading dysfunction where gut problems directly become brain problems — brain fog, anxiety, depression, and accelerated neurodegeneration.
This isn’t speculative anymore. A 2024 review in Nature Reviews Gastroenterology & Hepatology positioned the gut and brain barriers as bidirectional communication gates, where microbial signals directly influence blood-brain barrier permeability. And a 2019 Nature Medicine study found that blood-brain barrier breakdown is detectable as an early biomarker of cognitive dysfunction — often before other clinical signs appear.
If you’re experiencing unexplained cognitive issues alongside digestive problems, this connection is worth understanding.
The Short Version: Gut permeability allows lipopolysaccharide (LPS) from gram-negative bacteria into circulation, triggering the kynurenine pathway to produce neurotoxic quinolinic acid that directly damages the blood-brain barrier. Short-chain fatty acids (SCFAs) from beneficial gut bacteria protect both barriers by modulating tight junction proteins and reducing microglial inflammation. The vagus nerve provides a direct neural link between gut and brain that transmits inflammatory signals bidirectionally. Healing the gut barrier is the most effective way to protect the brain barrier. Key interventions: dietary changes to reduce inflammation, targeted probiotics that produce SCFAs and GABA, adequate fiber intake, and stress reduction.
The Parallel Barrier Systems
Your gut and brain are protected by barriers with remarkably similar architecture:
The intestinal barrier consists of a single layer of epithelial cells connected by tight junction proteins (claudins, occludin, zonula occludens). These tight junctions selectively allow nutrients through while blocking bacteria, toxins, and incompletely digested proteins.
The blood-brain barrier (BBB) consists of endothelial cells connected by tight junction proteins — many of the same protein families used in the gut. The BBB allows glucose, amino acids, and certain molecules through while blocking most pathogens, inflammatory mediators, and toxins.
Both barriers are dynamic, not static. They respond to signals from the immune system, microbiota, and neural activity. And critically, both break down through similar mechanisms: inflammatory cytokines degrade tight junction proteins, increasing permeability.
How a Leaky Gut Creates a Leaky Brain

The pathway from gut dysfunction to brain dysfunction is now well-characterized:
Step 1: Gut Barrier Breakdown
When the intestinal epithelial barrier is compromised — by chronic stress, processed food, alcohol, antibiotics, or infections — the tight junctions between epithelial cells loosen. This allows molecules that should stay in the gut lumen to leak into the bloodstream.
The key marker of this process is zonulin, a protein that modulates tight junction permeability. Elevated serum zonulin indicates increased gut permeability. Zonulin research shows that levels increase with age, correlating with inflammatory markers and metabolic dysfunction.
The biggest triggers of excessive zonulin release: bacterial overgrowth and gluten (specifically gliadin, in genetically susceptible individuals).
Step 2: LPS Enters Circulation
The most damaging molecule that escapes a leaky gut is lipopolysaccharide (LPS) — a component of gram-negative bacterial cell walls. In a healthy gut, LPS is contained within the gut lumen. When the barrier breaks down, LPS enters the bloodstream, creating a condition called metabolic endotoxemia.
Even low-level chronic LPS exposure triggers a systemic inflammatory response: elevated TNF-alpha, IL-1beta, IL-6, and other pro-inflammatory cytokines.
Step 3: The Kynurenine Pathway Cascade
A 2024 study clarified a critical intermediate step: circulating LPS activates the kynurenine pathway, which converts tryptophan (normally used for serotonin synthesis) into neurotoxic metabolites, particularly quinolinic acid. This is a double hit:
- Serotonin synthesis is reduced (tryptophan is diverted away from serotonin production)
- Quinolinic acid directly damages BBB endothelial cells and promotes excitotoxicity
This mechanism explains why gut problems so frequently co-occur with depression and anxiety — the kynurenine pathway shunt simultaneously depletes serotonin and produces neurotoxins.
Step 4: Blood-Brain Barrier Compromise
The inflammatory cytokines and LPS itself attack the BBB’s tight junction proteins through multiple mechanisms:
- Matrix metalloproteinase (MMP-9) activation: Inflammatory signals upregulate MMP-9, an enzyme that directly degrades tight junction proteins
- Caveolin-1 (Cav-1) phosphorylation: LPS induces phosphorylation of this membrane protein, increasing transcellular permeability
- Microglial activation: Once inflammatory signals reach the brain side of the BBB, they activate microglia (the brain’s immune cells), creating a neuroinflammatory cascade that further damages the barrier from the inside
Step 5: Neuroinflammation and Cognitive Dysfunction
With a compromised BBB, molecules that should never reach the brain — bacterial fragments, inflammatory cytokines, environmental toxins — now have access to vulnerable neurons. The result: neuroinflammation, oxidative stress, and progressive damage to neural circuits.
This manifests clinically as brain fog, impaired memory, anxiety, depression, and in severe or chronic cases, accelerated neurodegenerative disease. A 2019 Nature Medicine study found BBB breakdown detectable before clinical cognitive symptoms, establishing it as an early biomarker.
The Gut-Brain Axis: More Than Just Inflammation
The gut-brain connection operates through multiple parallel channels:
The Vagus Nerve
The vagus nerve is the primary neural highway connecting gut and brain. It carries both sensory information from the gut to the brain (afferent signals) and regulatory signals from the brain back to the gut (efferent signals). Approximately 80% of vagal fibers are afferent — meaning the gut is sending far more information to the brain than the other way around.
Gut bacteria directly influence vagal signaling. A 2025 study showed that GABA-producing probiotic strains (Lactiplantibacillus plantarum Lp815) reduced anxiety scores in 68% of participants, likely through vagal-mediated signaling from gut GABA production to the brain. See our GABA article for the full Lp815 trial data.
Short-Chain Fatty Acids (SCFAs)
When beneficial gut bacteria ferment dietary fiber, they produce short-chain fatty acids — primarily butyrate, propionate, and acetate. A 2025 review in Journal of Neuroinflammation detailed how SCFAs:
- Regulate microglial function: SCFAs modulate microglial activation, reducing neuroinflammation
- Strengthen both barriers: Butyrate upregulates tight junction protein expression in both intestinal epithelium and BBB endothelium
- Cross the BBB: SCFAs enter the brain and directly influence neurotransmitter synthesis and neuroinflammation
When dysbiosis (gut microbial imbalance) reduces SCFA-producing bacteria, both the gut and brain barriers lose this protective support simultaneously.
The Alpha-Synuclein Connection
Emerging research suggests that some neurodegenerative diseases may literally begin in the gut. A 2025 clinical study provided evidence that alpha-synuclein — the misfolded protein central to Parkinson’s disease — can be “dispatched” from the gut to the brain through the vagus nerve, amid inflammatory gut changes. This gut-origin hypothesis for Parkinson’s has gained significant support and may eventually reshape how we think about neurodegenerative disease prevention.
Conditions Linked to Gut-Brain Barrier Dysfunction
The gut-brain barrier connection has been implicated in:
- Depression: Kynurenine pathway activation depletes serotonin while producing neurotoxins; multiple studies show elevated LPS and gut permeability markers in depressive disorders
- Anxiety: Disrupted GABA signaling, neuroinflammation, and HPA axis dysregulation secondary to gut barrier dysfunction
- Alzheimer’s disease: BBB breakdown as an early biomarker; neuroinflammation from gut-derived endotoxemia accelerates amyloid pathology
- Parkinson’s disease: Alpha-synuclein gut-to-brain transmission; gut symptoms often precede motor symptoms by years
- Autism spectrum disorders: Altered intestinal permeability and BBB integrity documented in multiple studies
- Brain fog and cognitive impairment: The most common subjective complaint, reflecting subclinical neuroinflammation
Testing for Gut-Brain Barrier Dysfunction
If you suspect gut-brain barrier issues, these functional tests can provide data:
- Serum zonulin: Marker of intestinal permeability. Elevated levels indicate increased gut barrier leakage.
- Serum LPS/LPS-binding protein: Indicates metabolic endotoxemia from gut barrier compromise.
- Calprotectin (stool): Marker of intestinal inflammation. Elevated levels suggest active gut inflammation.
- MMP-9 (serum): Elevated levels suggest active tight junction degradation in gut and/or BBB.
- Comprehensive stool analysis: Identifies dysbiosis, pathogenic bacteria, and SCFA-producing bacteria levels.
These tests are available through functional medicine practitioners. They’re not definitive on their own but can guide targeted intervention.
Healing Both Barriers: What Works
The most effective approach is to address the gut first — because a healthy gut barrier automatically supports BBB integrity through reduced inflammation, increased SCFA production, and normalized immune signaling.
Dietary Interventions
Remove inflammatory triggers:
- Processed foods, refined sugar, and seed oils promote gut inflammation
- Alcohol directly damages intestinal epithelium
- Gluten triggers zonulin release in susceptible individuals (not everyone — celiac disease and non-celiac gluten sensitivity affect a subset of the population)
Add barrier-supporting foods:
- Fermented foods (kimchi, sauerkraut, yogurt, kefir): Provide both GABA and SCFA-producing bacteria
- High-fiber foods: Feed SCFA-producing bacteria. Aim for 25-35g daily from vegetables, legumes, and whole grains
- Bone broth: Contains glutamine, glycine, and collagen — amino acids that support epithelial repair
- Polyphenol-rich foods (berries, olive oil, dark chocolate): Anti-inflammatory and supportive of beneficial bacteria
- Omega-3-rich foods (fatty fish, walnuts): Anti-inflammatory effects on both barriers
Targeted Supplementation
- L-Glutamine (5-10g daily): The primary fuel for intestinal epithelial cells. Supports tight junction integrity and accelerates gut barrier repair. This is the single most evidence-backed gut-healing supplement.
- Butyrate (300-600mg daily, or tributyrin form): Directly upregulates tight junction proteins in both gut and BBB. Can also be increased through dietary fiber feeding beneficial bacteria.
- Probiotics: Strain-specific. GABA-producing strains (Lp815, L. rhamnosus JB-1) and SCFA-producing strains (Bifidobacterium longum, Lactobacillus acidophilus) have the best evidence.
- Curcumin (400-1,000mg enhanced bioavailability): Anti-inflammatory, reduces gut and brain inflammation through NF-kB and NLRP3 inflammasome inhibition.
- Omega-3s (2g+ EPA/DHA daily): Anti-inflammatory support for both barrier systems.
- Collagen peptides (10-15g daily): Provide amino acids (glycine, proline) that support epithelial repair.
- Digestive enzymes: If you have documented enzyme insufficiency, improving digestion reduces the antigenic load that damages the gut barrier.
Lifestyle Interventions
- Stress reduction: Cortisol directly increases intestinal permeability through corticotropin-releasing factor pathways. Meditation, yoga, and adequate sleep are not optional add-ons — they’re core to gut barrier integrity.
- Vagus nerve activation: Deep breathing exercises, cold water face immersion, humming/chanting, and meditation all stimulate vagal tone, enhancing the anti-inflammatory reflex. See our GABA article on how exercise and yoga increase brain GABA.
- Exercise (moderate intensity): Improves gut motility, increases microbial diversity, and reduces systemic inflammation. But overtraining can temporarily increase gut permeability — another reason to avoid excessive exercise intensity.
My Protocol
For gut-brain barrier support, my approach focuses on prevention rather than repair:
- Daily: High-fiber diet (30g+ from vegetables and legumes), 2-3 servings of fermented foods, omega-3s (2g from fish oil), 400mg curcumin (Longvida)
- Regular: Moderate exercise 5x/week, meditation 10-15 minutes morning, 8 hours sleep
- Avoided: Excessive alcohol, ultra-processed foods, chronic high-stress exposure without recovery
- Occasional: L-glutamine (5g) after periods of dietary indiscretion or travel (when gut disruption is common)
The overarching principle: your brain is only as healthy as your gut. The barriers that protect both organs share the same vulnerabilities and respond to the same interventions. Protect one and you protect both. Damage one and both suffer.