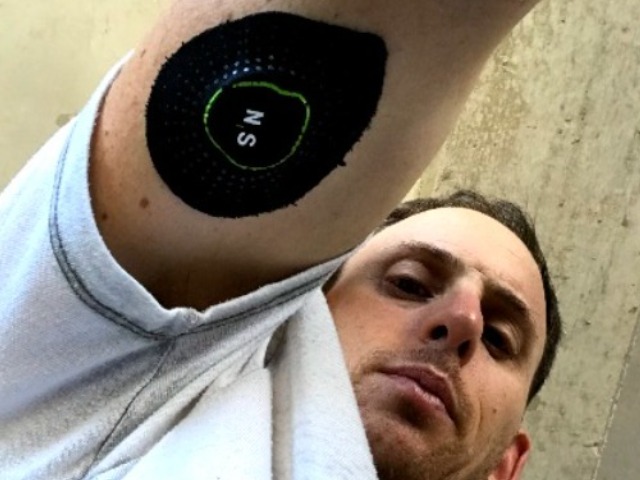
What gets measured gets managed. I’ve repeated this line to clients for years, but nothing drove it home quite like strapping a continuous glucose monitor to my arm and watching my blood sugar react to everything I ate, drank, and did for two straight weeks.
Blood sugar regulation is one of the most critical — and most overlooked — metrics in preventive health. It’s not just about diabetes risk. Glycemic variability affects your hormones, immune function, circulation, cognitive performance, and mood. If your blood sugar is on a rollercoaster all day, your energy, focus, and long-term health are along for the ride. And the frustrating reality is that standard blood work (fasting glucose, HbA1c) only gives you a snapshot. It tells you nothing about how your body actually responds to the specific foods you eat, the exercise you do, or the stress you experience.
That’s where continuous glucose monitoring comes in. I recently tested a Nutrisense CGM for 14 days, and it fundamentally changed how I think about my diet and metabolic health. Here’s the full breakdown.
Key Takeaways: A CGM tracks blood sugar in real time, revealing how your unique metabolism responds to specific foods and activities. Nutrisense pairs the hardware with an assigned dietitian who helps interpret your data — this is where the real value lives. Glycemic variability (not just fasting glucose) is now considered a more meaningful marker of metabolic health. Walking after meals and strategic supplementation with compounds like dihydroberberine are the simplest levers for improving glucose control.
What Is Continuous Glucose Monitoring?

A CGM is a small sensor that attaches to the back of your upper arm and tracks glucose levels continuously for 14 days. Unlike finger-prick tests that give you a single reading, a CGM captures the full picture — every spike, every dip, every recovery — and correlates it with your food intake, activity, sleep, and stress levels.
The insertion is painless (I barely felt it), and the device is waterproof, discreet, and stable enough that I frequently forgot it was there. You scan it with your phone to pull the data into the Nutrisense app, and from there you can start making connections between what you do and how your blood sugar responds.
Nutrisense specifically combines the CGM hardware with app-based data tracking and — critically — a personal dietitian assigned to your account. This human element is what separates it from just wearing a sensor and staring at numbers.
The CGM landscape shifted significantly in 2024 when the FDA cleared the first over-the-counter continuous glucose monitors for adults with and without diabetes. Dexcom’s Stelo became available without a prescription in summer 2024, followed by Abbott’s Lingo. This means CGMs are now more accessible than ever for metabolic health optimization — though the OTC options lack the dietitian support that makes Nutrisense’s offering uniquely actionable.
My 14-Day Experience
Getting Started
I’ll admit I was apprehensive before trying this. I didn’t know what to expect from the application process, and the idea of wearing a medical device on my arm for two weeks felt intrusive. Those concerns evaporated quickly.
Nutrisense sends clear instructions and short video tutorials. Application took about 30 seconds. Once attached, the sensor was completely stable — I showered, slept, and exercised without any interference. The device is remarkably stealthy; most people didn’t notice it under a sleeve.
The Learning Curve
The first 2-3 days are calibration time — the sensor needs to settle in and your initial readings may not be fully accurate. I used this period to get into the habit of logging everything: meals, snacks, workouts, stressful meetings, sleep quality.
This is the part that takes discipline. The value of a CGM is directly proportional to how diligently you track your inputs. Multiple times I forgot to log a meal or snack and had to backfill hours later, which meant some correlations were imprecise. It’s a small hassle, but the payoff in self-knowledge is enormous.
The Dietitian Makes the Difference
This is where Nutrisense truly earns its value. Almost daily, I received messages from my assigned dietitian commenting on my data and helping me understand what the metrics actually meant.
Some of the CGM metrics are genuinely confusing — even for someone immersed in the health optimization world. Standard deviation, mean glucose, time in range, glycemic variability — these numbers need context to be actionable. Having a professional translate the data into practical dietary adjustments was the difference between interesting data and meaningful behavior change.
What I Learned
Glycemic Variability Is the Real Metric
Here’s something most people don’t know: blood glucose fluctuations following meals are now considered a more meaningful indicator of metabolic health than HbA1c. Research published in PLOS Biology demonstrates that failure to control glycemic variability is an independent risk factor for diabetes and cardiovascular disease, indicating broader metabolic dysfunction.
The CGM measures this as “Standard Deviation” — you want yours below 14. This was a revelation for me. My fasting glucose was always fine on standard blood work, but the CGM revealed that certain meals were sending my blood sugar on wild rides that never showed up on routine tests.
A 2025 systematic review in Sensors confirmed that even in non-diabetic individuals, higher and prolonged glycemic excursions contribute to cardiovascular risk through increased inflammation, endothelial dysfunction, and oxidative stress — reinforcing that glucose variability within the “normal” range still matters. However, research from Mass General Brigham in 2024 found an important nuance: while CGM metrics correlate well with HbA1c in diabetic patients, this relationship weakens in prediabetes and disappears in people without diabetes. This means CGMs are most valuable as behavioral “biofeedback” tools for non-diabetics, showing how specific foods and activities impact real-time blood sugar, rather than as diagnostic instruments for long-term glucose control.
Glucose Peaks Tell You What’s Working
Ideally, your post-meal glucose peak should stay under 140 mg/dL. Every time you eat, your blood sugar rises — that’s normal. But the magnitude of the spike and how quickly you return to baseline tells you whether your insulin response is functional and whether that specific food works for your metabolism.
I discovered that certain foods I considered “healthy” (like some grain bowls and smoothies) were causing peaks well above 140, while other meals I’d been avoiding (higher-fat options) kept me remarkably stable. This kind of personalized data is impossible to get any other way.
Walking After Meals Is a Game-Changer
The simplest, most cost-effective intervention I discovered: a 10-15 minute walk after eating dramatically reduced my post-meal glucose spikes. This isn’t news to researchers, but seeing it in real time on my own data made it visceral and motivating. It’s now a non-negotiable habit.
A 2024 clinical trial from Heinrich-Heine University (the CGM-HYPE study) provided further granularity here: in healthy young adults wearing CGMs under standardized conditions, anaerobic exercise produced significantly greater glucose excursion compared to aerobic exercise, and food with rich carbohydrate content caused the highest glucose increases. This aligns with what I saw — the type and intensity of movement matters, not just whether you move at all.
Strategic Supplementation
Dihydroberberine is, in my experience, nature’s most effective tool for blood sugar control. I was already familiar with it, but the CGM let me actually quantify its impact on my post-meal glucose response. The difference was measurable and consistent.
For those looking to support metabolic health through supplementation, I’d also recommend exploring berberine (the parent compound), optimizing magnesium status (magnesium deficiency impairs insulin sensitivity), and being mindful of caffeine timing — I noticed that morning coffee on an empty stomach caused a meaningful glucose spike that disappeared when I ate something first.
Who Should Try a CGM?
A continuous glucose monitor isn’t just for diabetics. I’d recommend it for anyone who:
- Wants to understand how their unique metabolism responds to specific foods
- Is dealing with unexplained energy crashes, brain fog, or mood swings
- Is serious about longevity and metabolic health optimization
- Wants data-driven dietary guidance rather than generic nutrition advice
The 14-day commitment is enough to identify your biggest metabolic triggers and build habits around them. The insights carry forward long after you remove the sensor.
Bottom Line
Nutrisense gave me more actionable metabolic intelligence in two weeks than years of annual blood work. The combination of continuous monitoring, app-based tracking, and human dietitian support creates a feedback loop that genuinely changes behavior. It’s not cheap, but for anyone serious about metabolic health, the ROI in knowledge and habit formation is substantial.
The most important thing I took away: metabolic health is deeply personal. What spikes one person’s blood sugar may be perfectly fine for another. Generic dietary advice can only take you so far. If you want to truly optimize, you need your own data.
For more on blood sugar optimization and its connection to cognitive performance, check out our articles on blood sugar and cognition and the best natural alternatives to metformin.